Difference between revisions of "Contrast medium reaction"
(Wording) |
(+Lists) |
||
| Line 1: | Line 1: | ||
{{Authors|[[User:Mikael Häggström|Mikael Häggström]]}} | {{Authors|[[User:Mikael Häggström|Mikael Häggström]]}} | ||
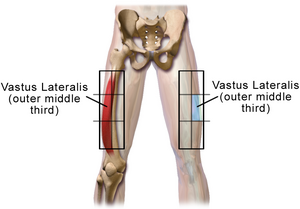
| − | + | [[File:Injection Sites Intramuscular Thigh Adult.png|thumb|Adrenaline injection site.]] | |
| − | {{Nutshell|In a more severe reaction: | + | {{Nutshell|In a more severe reaction:<ref name=SURF>Unless otherwise specified in lists and table: {{cite web|url=http://www.mastcellssjukdom.se/wp-content/uploads/2015/12/Nationella_rekommendationer_%C3%B6verk%C3%A4nslighetsreaktioner_kontrastmedel__PDF_2014-10-17.pdf|title=Hypersensitivity reactions against contrast media - Swedish Society of Uroradiology [Swedish: Överkänslighetsreaktioner mot kontrastmedel – SURFs kontrastmedelsgrupp] ], 2014-10-17}}</ref> |
| − | + | *'''Adrenaline''', 0.3-0.5mg in adults, given intramuscularly. | |
*Summon an '''anesthesiologist''' | *Summon an '''anesthesiologist''' | ||
| − | |||
}}<br clear="all"> | }}<br clear="all"> | ||
In case of a '''contrast medium reaction''', anaphylaxis is a more severe allergic reaction whose diagnostic criteria generally include low blood pressure and/or respiratory distress.<ref name="KimFischer2011">{{cite journal|last1=Kim|first1=Harold|last2=Fischer|first2=David|title=Anaphylaxis|journal=Allergy, Asthma & Clinical Immunology|volume=7|issue=Suppl 1|year=2011|pages=S6|issn=1710-1492|doi=10.1186/1710-1492-7-S1-S6}}</ref> In anaphylaxis, intramuscularly administered adrenaline is the most important initial therapy.<ref name=SURF/> Also, an '''anesthesiologist''' or corresponding clinician on duty should be summoned. A '''peripheral venous catheter''' is needed for the administration of IV fluids.<ref name=SURF/> '''Oxygen saturation''', '''pulse''' and '''blood pressure''' are monitored.<ref name=SURF/> | In case of a '''contrast medium reaction''', anaphylaxis is a more severe allergic reaction whose diagnostic criteria generally include low blood pressure and/or respiratory distress.<ref name="KimFischer2011">{{cite journal|last1=Kim|first1=Harold|last2=Fischer|first2=David|title=Anaphylaxis|journal=Allergy, Asthma & Clinical Immunology|volume=7|issue=Suppl 1|year=2011|pages=S6|issn=1710-1492|doi=10.1186/1710-1492-7-S1-S6}}</ref> In anaphylaxis, intramuscularly administered adrenaline is the most important initial therapy.<ref name=SURF/> Also, an '''anesthesiologist''' or corresponding clinician on duty should be summoned. A '''peripheral venous catheter''' is needed for the administration of IV fluids.<ref name=SURF/> '''Oxygen saturation''', '''pulse''' and '''blood pressure''' are monitored.<ref name=SURF/> | ||
| Line 10: | Line 9: | ||
In general in a contrast medium reaction, the patient should be evaluated for the presence of the following symptoms and be medicated accordingly.<ref name=SURF/> | In general in a contrast medium reaction, the patient should be evaluated for the presence of the following symptoms and be medicated accordingly.<ref name=SURF/> | ||
| + | ==Evaluation== | ||
| + | Initial evaluation can be done according to an ABCDE approach:<ref name=SURF/> | ||
| + | * Airway: Stridor? Swollen tongue? | ||
| + | * Breathing: Cyanosis? Use pulse oximeter if available. | ||
| + | * Circulation: Palpable pulse over radial, femoral and carotid artery? Heart rate? Blood pressure? Difficulty in taking blood pressure must not delay adrenaline administration. | ||
| + | * Disability: Altered level of consciousness? | ||
| + | * Exposure: Hives? | ||
| + | |||
| + | ==In severe hives and progressive angioedema<ref name=SURF/>== | ||
| + | [[File:Angioedema2010.JPG|thumb|Angioedema]] | ||
| + | * 0,3-0,5 mg adrenaline intramuscularly on the anterolateral part of the mid-thigh. It is repeated if needed every | ||
| + | 3–5 minutes. | ||
| + | * Corticosteroid (see Table of medications below) | ||
| + | * Observation at least 30 minuter | ||
| + | |||
| + | ==Anaphylaxis<ref name=SURF/>== | ||
| + | * 0,3-0,5 mg adrenaline intramuscularly on the anterolateral part of the mid-thigh. It is repeated if needed every | ||
| + | 3–5 minutes. | ||
| + | * Summon anesthesiologist or corresponding clinician on duty | ||
| + | * Oxygen, 10 L/min on mask. Attach a pulse oximeter. | ||
| + | * In asthma or bronchospasm: Salbutamol inhalations (see Table of medications below) | ||
| + | * In hypotension: Tilt the table to lower the head of the patient and give volume expander | ||
| + | * Corticosteroid (see Table of medications below) | ||
| + | |||
| + | ==Cardiac arrest (unconscious and no breathing)<ref name=SURF/>== | ||
| + | [[File:Chest compressions.gif|thumb|Chest compressions.]] | ||
| + | * Start CPR: 100 chest compressions per minute and ventilate x2 every 30 compressions | ||
| + | * Connect a defibrillator | ||
| + | * If ventricular fibrillation or tachycardia: defibrillate at 200 Joule | ||
| + | * If asystole or pulseless electrical activity (PEA): 1 mg adrenaline 0,1 i.v. bolus | ||
| + | * Continue CPR | ||
| + | |||
| + | ==Itching hives== | ||
| + | If ABCDE is otherwise normal:<ref name=SURF/> | ||
| + | * Antihistamine (see Table of medications below) | ||
| + | * Observation at least 30 minutes | ||
| + | |||
| + | ==Table of medications== | ||
{|class="wikitable" | {|class="wikitable" | ||
!rowspan=2| Symptoms<ref name=SURF/> !!rowspan=2| Medication<ref name=SURF/> !!rowspan=2| Route<ref name=SURF/> !!colspan=2| Dosage<ref name=SURF/> !!rowspan=2| Time to effect<ref name=SURF/> ||rowspan=2| Repeat<ref name=SURF/> | !rowspan=2| Symptoms<ref name=SURF/> !!rowspan=2| Medication<ref name=SURF/> !!rowspan=2| Route<ref name=SURF/> !!colspan=2| Dosage<ref name=SURF/> !!rowspan=2| Time to effect<ref name=SURF/> ||rowspan=2| Repeat<ref name=SURF/> | ||
Revision as of 22:51, 22 May 2018
Author:
[notes 1]
In a more severe reaction:[1]
|
In case of a contrast medium reaction, anaphylaxis is a more severe allergic reaction whose diagnostic criteria generally include low blood pressure and/or respiratory distress.[2] In anaphylaxis, intramuscularly administered adrenaline is the most important initial therapy.[1] Also, an anesthesiologist or corresponding clinician on duty should be summoned. A peripheral venous catheter is needed for the administration of IV fluids.[1] Oxygen saturation, pulse and blood pressure are monitored.[1]
In general in a contrast medium reaction, the patient should be evaluated for the presence of the following symptoms and be medicated accordingly.[1]
Contents
Evaluation
Initial evaluation can be done according to an ABCDE approach:[1]
- Airway: Stridor? Swollen tongue?
- Breathing: Cyanosis? Use pulse oximeter if available.
- Circulation: Palpable pulse over radial, femoral and carotid artery? Heart rate? Blood pressure? Difficulty in taking blood pressure must not delay adrenaline administration.
- Disability: Altered level of consciousness?
- Exposure: Hives?
In severe hives and progressive angioedema[1]
- 0,3-0,5 mg adrenaline intramuscularly on the anterolateral part of the mid-thigh. It is repeated if needed every
3–5 minutes.
- Corticosteroid (see Table of medications below)
- Observation at least 30 minuter
Anaphylaxis[1]
- 0,3-0,5 mg adrenaline intramuscularly on the anterolateral part of the mid-thigh. It is repeated if needed every
3–5 minutes.
- Summon anesthesiologist or corresponding clinician on duty
- Oxygen, 10 L/min on mask. Attach a pulse oximeter.
- In asthma or bronchospasm: Salbutamol inhalations (see Table of medications below)
- In hypotension: Tilt the table to lower the head of the patient and give volume expander
- Corticosteroid (see Table of medications below)
Cardiac arrest (unconscious and no breathing)[1]
- Start CPR: 100 chest compressions per minute and ventilate x2 every 30 compressions
- Connect a defibrillator
- If ventricular fibrillation or tachycardia: defibrillate at 200 Joule
- If asystole or pulseless electrical activity (PEA): 1 mg adrenaline 0,1 i.v. bolus
- Continue CPR
Itching hives
If ABCDE is otherwise normal:[1]
- Antihistamine (see Table of medications below)
- Observation at least 30 minutes
Table of medications
| Symptoms[1] | Medication[1] | Route[1] | Dosage[1] | Time to effect[1] | Repeat[1] | |
|---|---|---|---|---|---|---|
| Adults | Children | |||||
|
Injection of adrenaline | Intramuscular in lateral thigh | 0.3 - 0.5 mg |
|
Less than 5 min | Every 5-10 min if needed |
| Asthma | Salbutamol (Ventolin) or own bronchodilator | Inhalation |
|
|
Less than 5 min | Every 10 mins if needed |
| Hypoxia | Oxygen | Mask | >5 l/min | Almost immediate | Continuous | |
| Altered level of consciousness or hypotension | Volume expander such as Ringer's | IV with pressure | 20mg/kg | Fast | As needed | |
| All anaphylaxis cases | Antihistamine such as desloratadine (Clarinex/Aerius) | Oral | 10mg of desloratadine |
|
Within 30-60 minutes | Usually not |
| All anaphylaxis cases | Glucocorticoid such as betamethasone | Oral or IV |
|
|
2-3 hours | Usually not |
References
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 1.11 1.12 1.13 1.14 1.15 Unless otherwise specified in lists and table: . Hypersensitivity reactions against contrast media - Swedish Society of Uroradiology [Swedish: Överkänslighetsreaktioner mot kontrastmedel – SURFs kontrastmedelsgrupp ], 2014-10-17].
- ↑ Kim, Harold; Fischer, David (2011). "Anaphylaxis ". Allergy, Asthma & Clinical Immunology 7 (Suppl 1): S6. doi:. ISSN 1710-1492.
Cite error: <ref> tags exist for a group named "notes", but no corresponding <references group="notes"/> tag was found, or a closing </ref> is missing