Difference between revisions of "X-ray of knee prosthesis"
m (→Report: Opposed) |
(→Follow-up: +Zones) |
||
| Line 25: | Line 25: | ||
===Radiolucent lines=== | ===Radiolucent lines=== | ||
| − | Radiolucent lines may indicate loosening of the implant. A radiolucent line thinner than than 2 mm can be tolerated at the cement-bone interface (for cemented implants) or implant-bone interface (for cementless implants) if it remains stable and appears within the first 6 months (cemented implants) or the first 2 years (cementless implants) after surgery.<ref name="Cyteval2016">{{cite journal|last1=Cyteval|first1=C.|title=Imaging of knee implants and related complications|journal=Diagnostic and Interventional Imaging|volume=97|issue=7-8|year=2016|pages=809–821|issn=22115684|doi=10.1016/j.diii.2016.02.015}}</ref> | + | [[File:Knee prosthesis zones by Knee Society 2015, lateral view.jpg|thumb|150px|KS (Knee Society) zones, for localizing radiolucent zones or other focal changes.<ref name="MeneghiniMont2015">{{cite journal|last1=Meneghini|first1=R. Michael|last2=Mont|first2=Michael A.|last3=Backstein|first3=David B.|last4=Bourne|first4=Robert B.|last5=Dennis|first5=Doug A.|last6=Scuderi|first6=Giles R.|title=Development of a Modern Knee Society Radiographic Evaluation System and Methodology for Total Knee Arthroplasty|journal=The Journal of Arthroplasty|volume=30|issue=12|year=2015|pages=2311–2314|issn=08835403|doi=10.1016/j.arth.2015.05.049}}</ref>]] |
| + | [[File:Knee prosthesis zones by Knee Society 2015, AP view.jpg|thumb|180px|KS zones, AP view.<ref name="MeneghiniMont2015"/>]] | ||
| + | Radiolucent lines may indicate loosening of the implant. A radiolucent line thinner than than 2 mm can be tolerated at the cement-bone interface (for cemented implants) or implant-bone interface (for cementless implants) if it remains stable and appears within the first 6 months (cemented implants) or the first 2 years (cementless implants) after surgery.<ref name="Cyteval2016">{{cite journal|last1=Cyteval|first1=C.|title=Imaging of knee implants and related complications|journal=Diagnostic and Interventional Imaging|volume=97|issue=7-8|year=2016|pages=809–821|issn=22115684|doi=10.1016/j.diii.2016.02.015}}</ref> There are various classification systems for specifying the location of radiolucent spaces,<ref name="NapierO’Neill2018">{{cite journal|last1=Napier|first1=Richard J.|last2=O’Neill|first2=Christopher|last3=O’Brien|first3=Seamus|last4=Doran|first4=Emer|last5=Mockford|first5=Brian|last6=Boldt|first6=Jens|last7=Beverland|first7=David E.|title=A prospective evaluation of a largely cementless total knee arthroplasty cohort without patellar resurfacing: 10-year outcomes and survivorship|journal=BMC Musculoskeletal Disorders|volume=19|issue=1|year=2018|issn=1471-2474|doi=10.1186/s12891-018-2128-1}}</ref><ref name="KumarYadav2014">{{cite journal|last1=Kumar|first1=Nishikant|last2=Yadav|first2=Chandrashekhar|last3=Raj|first3=Rishi|last4=Anand|first4=Sumit|title=How to Interpret Postoperative X-rays after Total Knee Arthroplasty|journal=Orthopaedic Surgery|volume=6|issue=3|year=2014|pages=179–186|issn=17577853|doi=10.1111/os.12123}}</ref> including by KS (Knee Society) zones published in 2015.<ref name="MeneghiniMont2015"/> | ||
===Displacement=== | ===Displacement=== | ||
Revision as of 17:56, 24 July 2019
Author:
Mikael Häggström [notes 1]
Contents
Post-operative evaluation

Knee replacement is evaluated by the following measures:
HKA: Hip-knee-ankle angle, which is ideally between 3° varum to 3° valgum from a right angle.[2]
- FFC: frontal femoral component angle. It is typically regarded as optimal when being 2–7° in valgus.[3]
- FTC: frontal tibial component angle, which is regarded as optimal when being at a right angle. A varus position of more than 3° has generally been found to increase the failure rate of the prosthesis.[3]- Anterior femoral notching (the femoral component causing reduced thickness of the distal femur anteriorly), seems to cause an increased risk of fractures when exceeding about 3 mm.[4]
- LTC: lateral (or sagittal) tibial component angle, which is ideally positioned so that the tibia is 0–7° flexed compared to at a right angle with the tibial plate.[3]
Report
In Swedish healthcare[5], the numbers of the angles are not reported if being within normal limits. Example of an normal case:
- Postoperative images of knee implant in unremarkable position.
Also, unless you know the referring physician is familiar with the same angle terminology, preferably report any deviating angles as varus/valgus deviation or ventral/dorsal angulation, such as:
- An abnormally increased valgus angulation of __° of the femur component in relation to femoral diaphysis.
- A abnormal ventral angulation of __° of the tibial diaphysis in relation to the tibial component.
- See also: General notes on reporting
Follow-up
Potential complications that need to be evaluated on follow-up are as follows.
Radiolucent lines
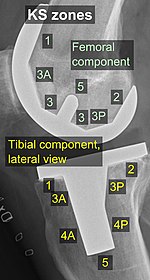

Radiolucent lines may indicate loosening of the implant. A radiolucent line thinner than than 2 mm can be tolerated at the cement-bone interface (for cemented implants) or implant-bone interface (for cementless implants) if it remains stable and appears within the first 6 months (cemented implants) or the first 2 years (cementless implants) after surgery.[7] There are various classification systems for specifying the location of radiolucent spaces,[8][9] including by KS (Knee Society) zones published in 2015.[6]
Displacement
A change in position is indicated by a significant change in either of the angles listed in the post-operative evaluation section above.[7]
Infection
Signs of infection include:[7]
- Rapidly progressing radiolucency and/or osteolysis
- Periosteal reaction
- Bubbles of air within soft tissue or fluid collection.
Other complications
- Fractures of prosthesis components.
- Wear of the polyethylene insert, which is the case when progressive thinning occurs over time.
- Dissociation of the polyethylene insert from the patellar component or tibial baseplate.
Reporting
In Swedish healthcare[10], an example report of a normal case may be:
- No changes since previous images on <date>.
- See also: General notes on reporting
Notes
- ↑ For a full list of contributors, see article history. Creators of images are attributed at the image description pages, seen by clicking on the images. See Radlines:Authorship for details.
References
- ↑ S.G.F. Abram, A.G Marsh, F. Nicol, A.S. Brydone, A. Mohammed, S.J. Spencer (2018-02-21). "The Impact Of Tibial Component Overhang On Outcome Scores And Pain In Total Knee Replacement ". Orthopaedic Proceedings.
- ↑ Inui, Hiroshi; Taketomi, Shuji; Nakamura, Kensuke; Takei, Seira; Takeda, Hideki; Tanaka, Sakae; Nakagawa, Takumi (2013). "Influence of navigation system updates on total knee arthroplasty ". Sports Medicine, Arthroscopy, Rehabilitation, Therapy & Technology 5 (1): 10. doi:. ISSN 1758-2555. PMID 23638774. (CC-BY-2.0)
- ↑ 3.0 3.1 3.2 Gromov, Kirill; Korchi, Mounim; Thomsen, Morten G; Husted, Henrik; Troelsen, Anders (2014). "What is the optimal alignment of the tibial and femoral components in knee arthroplasty? ". Acta Orthopaedica 85 (5): 480–487. doi:. ISSN 1745-3674. PMID 25036719.
- ↑ Lee, Ju Hong; Wang, Seong-Il (2015). "Risk of Anterior Femoral Notching in Navigated Total Knee Arthroplasty ". Clinics in Orthopedic Surgery 7 (2): 217. doi:. ISSN 2005-291X.
- ↑ NU Hospital Group, Sweden, Sep 2018
- ↑ 6.0 6.1 6.2 Meneghini, R. Michael; Mont, Michael A.; Backstein, David B.; Bourne, Robert B.; Dennis, Doug A.; Scuderi, Giles R. (2015). "Development of a Modern Knee Society Radiographic Evaluation System and Methodology for Total Knee Arthroplasty ". The Journal of Arthroplasty 30 (12): 2311–2314. doi:. ISSN 08835403.
- ↑ 7.0 7.1 7.2 Cyteval, C. (2016). "Imaging of knee implants and related complications ". Diagnostic and Interventional Imaging 97 (7-8): 809–821. doi:. ISSN 22115684.
- ↑ Napier, Richard J.; O’Neill, Christopher; O’Brien, Seamus; Doran, Emer; Mockford, Brian; Boldt, Jens; Beverland, David E. (2018). "A prospective evaluation of a largely cementless total knee arthroplasty cohort without patellar resurfacing: 10-year outcomes and survivorship ". BMC Musculoskeletal Disorders 19 (1). doi:. ISSN 1471-2474.
- ↑ Kumar, Nishikant; Yadav, Chandrashekhar; Raj, Rishi; Anand, Sumit (2014). "How to Interpret Postoperative X-rays after Total Knee Arthroplasty ". Orthopaedic Surgery 6 (3): 179–186. doi:. ISSN 17577853.
- ↑ NU Hospital Group, Sweden, Oct 2018


