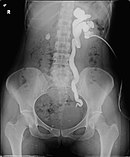
Antegrade pyelography
Author:
Mikael Häggström [notes 1]
Contents
Preparation
The procedure can be started in supine position. It can be done in a clean technique (not necessarily sterile) with gloves and radiation protection.
- Generally use low radiation dose fluoroscopy with normal dose single projections.
- Close any bladder catheter in order to easier detect any contrast ending up in the bladder.
Procedure with established nephrostomy
- Take an initial anteroposterior image including the presumed locations of the kidney, ureter and urinary bladder.
- Inject iodinated contrast, usually at least a volume corresponding to about 15 ml of 240mg/ml iodine. Observe both the imaging and whether the patient develops flank pain. Optionally, note how much contrast has been injected at that point.
- Note the following:
- Location of the tip of the catheter in the kidney
- Any visible hydronephrosis or hydroureter. If present, also note:
- Severity of the hydronephrosis (see section below)
- Any caliber change, or most distal part reached by contrast.
- Any contrast outside the catheter or urinary tract, including leakage along the outside of the catheter
- Flow into the urinary bladder (see below if none).
After the procedure, open up any closed bladder catheter.
If contrast does not reach the urinary bladder
Inject as much contrast as still comfortable by the patient. Observe the most distal part reached by contrast, and the shape thereof. Zooming in on this segment may detect subtle passage. Also turn your eye to the nephrostomy for leakage.
Obtain new projections after:
- Having the patient in a more standing position.
- Having the patient cough.
Hydronephrosis grading
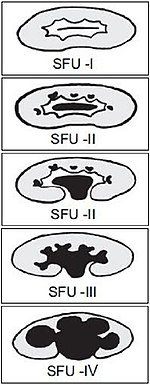
The Society of Fetal Ultrasound has developed a grading system for hydronephrosis, initially intended for use in neonatal and infant hydronephrosis, but it is now used for grading hydronephrosis in adults as well:[1]
- Grade 0 – No renal pelvis dilation. Cutoff values for different patient populations are:
- Fetuses: An anteroposterior diameter of less than 4 mm in fetuses up to 32 weeks of gestational age and 7 mm afterwards.[2]
- Adults, defineddifferently by different sources, with anteroposterior diameters ranging between 10 and 20 mm.[3] About 13% of normal healthy adults have a transverse pelvic diameter of over 10 mm.[4]
- Pregnant women in the last two trimesters: The maximum normal expected renal pelvic diameter (97.5 percent prediction interval) is 27 mm on the right and 18 mm on the left.[5]
- Grade 1 (mild) – Mild renal pelvis dilation (anteroposterior diameter less than 10 mm in fetuses[2]) without dilation of the calyces nor parenchymal atrophy
- Grade 2 (mild) – Moderate renal pelvis dilation (between 10 and 15 mm in fetuses[2]), including a few calyces
- Grade 3 (moderate) – Renal pelvis dilation with all calyces uniformly dilated. Normal renal parenchyma
- Grade 4 (severe) – As grade 3 but with thinning of the renal parenchyma
In Swedish practice,[notes 2] the most important is a subjective classification into mild, moderate or severe, with optional mention of numerical grade (unless specifically requested in the referral).
Report
The report may be a chronological description of the procedure, and should include:
- Catheter tip location
- Any visible hydronephrosis or hydroureter
- If present, grading of any hydronephrosis
- Location of the most distal part reached by contrast, or caliber change
- Even absence of leakage
Optionally also:
- If obstructed:
- Classification as partial or complete (that is, some or no passage of contrast)
- Shape of the ureter at the obstruction.
- Correlation to findings on previous imaging such as CT
- Volume of contrast injected.
- Provocation with standing or coughing.
|
The tip of the nephrostomy is located in an inferior calyx. |
- See also: General notes on reporting
Notes
- ↑ For a full list of contributors, see article history. Creators of images are attributed at the image description pages, seen by clicking on the images. See Radlines:Authorship for details.
- ↑ NU Hospital Group, Sweden
References
- ↑ Laurence S Baskin. Overview of fetal hydronephrosis. Version Version 29.0. UpToDate. Retrieved on 2017-04-25. Last updated Apr 20, 2017
- ↑ 2.0 2.1 2.2 Page 189 in: V. D'Addario (2014). Donald School Basic Textbook of Ultrasound in Obstetrics & Gynecology . JP Medical Ltd. ISBN 9789351523376.
- ↑ Page 78 in: Justin Bowra, Russell E (2011). Emergency Ultrasound Made Easy, Edition 2 . Elsevier Health Sciences. ISBN 9780702048722.
- ↑ "Sonographic evaluation of renal appearance in 665 adult volunteers. Correlation with age and obesity ". Acta Radiol 34 (5): 482–5. 1993. doi:. PMID 8369185.
- ↑ Erickson, L. M.; Nicholson, S. F.; Lewall, D. B.; Frischke, Lauraline (1979). "Ultrasound evaluation of hydronephrosis of pregnancy ". Journal of Clinical Ultrasound 7 (2): 128–132. doi:. ISSN 00912751.
- ↑ Efe, Erkan; Bakacak, Murat; Serin, Salih; Kolus, Eyüp; Ercan, Önder; Resim, Sefa (2014). "Hormonal Treatment for Severe Hydronephrosis Caused by Bladder Endometriosis ". Case Reports in Urology 2014: 1–5. doi:. ISSN 2090-696X.